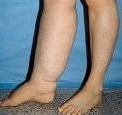
 Although we don’t often talk about it, Lymphedema is a common side effect of the surgery that many metastatic melanoma or non-melanoma skin cancer patients receive to remove nodal disease. It affects men and women, and can be uncomfortable and often painful, affecting daily activity.
Although we don’t often talk about it, Lymphedema is a common side effect of the surgery that many metastatic melanoma or non-melanoma skin cancer patients receive to remove nodal disease. It affects men and women, and can be uncomfortable and often painful, affecting daily activity.
Most often, lymphedema affects the arms and legs, however, lymphedema can also occur in other parts of the body, including the head and neck.
Despite best efforts to prevent it, I myself was the lucky recipient of a lymphedema diagnosis in 2014 after CLND (Completion Lymph Node Dissection) surgery in my right groin following stage IIIB nodular melanoma diagnosis. To this day I am learning how to cope with this condition which affects my right upper leg, and through this research I found a supportive group right here in B.C. – British Columbia Lymphedema Association – and they work with similar groups across Canada. Please see below for a full list of Lymphedema contacts in your area.
“Lymphedema is the abnormal buildup of fluid in soft tissue due to a blockage in the lymphatic system. The lymphatic system helps fight infection and other diseases by carrying lymph, a colorless fluid containing white blood cells, throughout the body using a network of thin tubes called vessels. Small glands called lymph nodes filter bacteria and other harmful substances out of this fluid. However, when the lymph nodes are removed or damaged, lymphatic fluid collects in the surrounding tissues, causing them to swell. Lymphedema may develop immediately after surgery or radiation therapy, or it may occur months or even years after cancer treatment has ended.” (Source)
People with lymphedema in an arm or leg may experience the following symptoms:
- Swelling that begins in the arm or leg matching the quarter of the body treated for cancer
- “Heavy” feeling in the arm or leg
- Weakness or decreased flexibility
- Rings, watches, or clothes that become too tight
- Discomfort or pain, although often there is no pain
- Tight, shiny, warm, or red skin
- Skin that does not indent at all when pressed, or hardened skin
- Thicker skin (hyperkeratosis)
Estimates from recent Canadian sources indicate that approximately 1 million Canadians have the incurable disease, many unaware of the true cause of their swelling which is often misinterpreted as fat. There are many causes of lymphedema. Lymphedema appears in two forms; a categorization based on the initial cause either primary or secondary.
Secondary lymphedema, presenting as swollen, heavy limb(s) and an immune system that can’t do its job, results from post trauma damage to the lymphatic system. Secondary Lymphedema can be triggered by accidents, injuries and cancer-related surgeries such as CLND (Completion Lymph Node Dissection) other non cancer surgeries, cellulitis infection, obesity & prolonged edema from other causes such as heart failure all of which can damage lymph nodes and lymphatic channels.
Primary lymphedema is less common but can occur at any stage in life from birth through to mid 50’s, a common age of onset. To read more about these types of Lymphedema, please visit BC Lymphedema Association – What is Lymphedema
Treatment of Lymphedema should be done by a Health Care Professional (HCP) who has been trained in the care of lymphedema/lipedema/lymphatic pathologies. Treatment may be with Combined Decongestive Therapy (CDT), CDT consists of Manual Lymph Drainage, Skin Care, Compression and Exercise. Or, it may be possible to use compression alone, under the supervision of a trained HCP.
There are a lot of things that a person, especially cancer survivors could do to ensure that lymphedema is delayed or the severity is reduced. The goal of the BC Lymphedema Association (BCLA) is to provide information and support for those newly diagnosed, uncertain about what is happening to them and where to turn for help. The majority of the medical profession know very little about lymphedema or how to treat it.
BCLA is a resource to help patients find therapist, fitters, and suppliers & learn more about how to manage their condition. For more information and to join in their World Lymphedema Day awareness events visit their website www.bclymph.org.
And in other provinces, please see the following:
Alberta Lymphedema Association – Alberta Lymphedema Association
Atlantic Clinical Lymphedema Network – About ACLN – Atlantic Clinical Lymphedema NetworkAtlantic Clinical Lymphedema Network (atlanticlymph.ca)
Lymphedema Association of Manitoba – Lymphedema Association of Manitoba (lymphmanitoba.ca)
Lymphedema Association of New Brunswick – Lymphedema Association of NB – Home | Facebook
Lymphedema Association of Newfoundland and Labrador – Lymphedema Association of Newfoundland and Labrador (lymphnl.com)
Lymphedema Association of Nova Scotia – Lymphedema Association Of Nova Scotia (lymphedemanovascotia.com)
Lymphedema Association of Ontario – Lymphedema Association of Ontario – Home (lymphontario.ca)
Lymphedema Association of Quebec – Lymphoedeme Lymphedema Association Quebec – Infolympho
Lymphedema Association of Saskatchewan – LAS – Lymphedema Association of Saskatchewan (sasklymph.ca)



