Merkel cell carcinoma (MCC) is a rare form of skin cancer, making up fewer than 1% of all non-melanoma skin cancers (Canadian Cancer Society, “Merkel Cell Carcinoma”). It manifests as malignant cells that form in the upper layer of skin, near the nerve endings that sense touch (Merck-Pfizer Alliance, “Merkel Cell Carcinoma Fact Sheet”). Merkel cell carcinoma often appears on sun-exposed areas of the skin, such as the legs, arms, neck, and head, as a blue or red lump on the skin. It most frequently occurs in fair-skinned males over 50 years of age (Merck-Pfizer Alliance).
Merkel cell carcinoma has a higher mortality rate than melanoma, with a mortality rate of 33% within five years of diagnosis (all stages) (Merck-Pfizer Alliance). Due to low awareness of merkel cell carcinoma, late diagnosis often results in the disease having reached stage III or IV(Merck-Pfizer Alliance).
Current treatment options for merkel cell carcinoma include chemotherapy, radiotherapy and surgery. These treatments are generally ineffective for advanced stage merkel cell carcinoma, resulting in a mortality rate of roughly 80% for stage IV metastatic merkel cell carcinoma patients (Merck-Pfizer Alliance). There is a gap in treatments for merkel cell carcinoma, and a need for more research and the staging of clinical trials to fill that gap.
Fortunately, at least one new treatment is in the works. JAVELIN merkel 200 is the title of an ongoing clinical study investigating the effects of avelumab, a treatment jointly manufactured by pharmaceutical developers Merck (Germany) and Pfizer (USA), on pre-treated patients with merkel cell carcinoma. The treatment inhibits PD-L1 interactions (Pharmaceutical Technology, “Merck and Pfizer’s Avelumab gets Breakthrough Status for Merkel Cell Carcinoma”), acting as an immune checkpoint inhibitor. The trial produced the largest set of data, in this patient population, of any anti-PD-L1/PD-1 (Pfizer, “ASCO 2016: Pivotal Avelumab Study Shows Positive Results in Metastatic Merkel Cell Carcinoma”). The results reported at the 52nd annual American Society of Clinical Oncology (ASCO) in Chicago this past June were promising: of 88 patients, 28 (31.8%) demonstrated an objective response rate during the Phase II study of avelumab (Pfizer). Of those that responded, 8 (9.1%) achieved complete responses, with 20 (22.7%) achieving partial responses (Pfizer). Of the entire trial, 62 (70.5%) patients experienced treatment related adverse effects (AEs), with the most common being fatigue (23.9% of patients) and infusion-related reactions (17%), with four patients (4.5%) experiencing grade 3 side effects and zero with grade 4 side effects (Pfizer). The ages of the trial participants ranged from 33-88 years old, and every participant had been pre-treated with chemotherapy (Pfizer). The patients received 10mg/kg of treatment intravenously every two weeks (Pfizer).
While avelumab is still in the trial stage, if it is approved, it will be the first approved treatment for Merkel Cell Carcinoma. Current information about the status of the trial can be found on the American clinical trial database or Pfizer’s website.
Works Cited:
Canadian Cancer Society, “Merkel Cell Carcinoma”.
Merck-Pfizer Alliance, “Merkel Cell Carcinoma Fact Sheet”.
Pfizer, “ASCO 2016: Pivotal Avelumab Study Shows Positive Results in Metastatic Merkel Cell Carcinoma”.
Pharmaceutical Technology, “Merck and Pfizer’s Avelumab gets Breakthrough Status for Merkel Cell Carcinoma”.









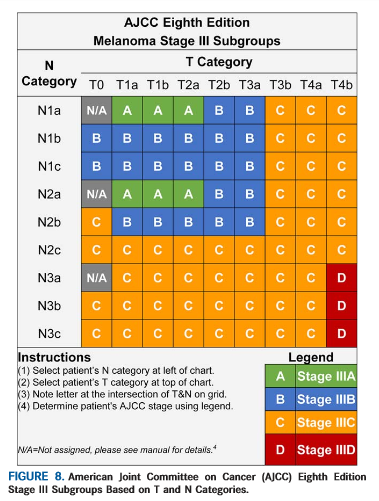 Staging is commonly used in melanoma diagnosis and treatment to indicate the advancement and severity and cancer in a patient. Melanoma stages range between 0-IV based on the TNM (tumour, nodes, metastasis) system. The
Staging is commonly used in melanoma diagnosis and treatment to indicate the advancement and severity and cancer in a patient. Melanoma stages range between 0-IV based on the TNM (tumour, nodes, metastasis) system. The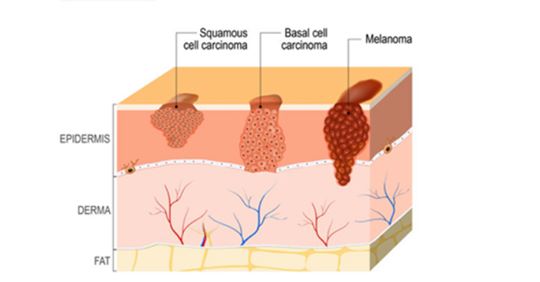 There are several different routes to being diagnosed with melanoma. The first step is generally a physical screening, during which your physician will check your skin for moles or other abnormalities and ask questions, such as if there have been any changes in your skin or moles, or the length of time you have had certain moles. In order to accurately answer these questions, it helps to self-examine your skin monthly to keep track of any changes; more information on moles and skin self-examinations can be found
There are several different routes to being diagnosed with melanoma. The first step is generally a physical screening, during which your physician will check your skin for moles or other abnormalities and ask questions, such as if there have been any changes in your skin or moles, or the length of time you have had certain moles. In order to accurately answer these questions, it helps to self-examine your skin monthly to keep track of any changes; more information on moles and skin self-examinations can be found 